Lymphatic Disorders
Understanding and Management of Disorders
of the Lymphatic System
The Lymphatic System
Lymphatic Vessels
The Lymphatic Vessels are also part of the circulatory system and are responsible for the return of lymph back into the bloodstream. Lymph consists of the fluid that escapes from blood vessels and accumulates between cells, as well as external agents (microorganisms and toxic substances) that may be found in the intercellular space due to injury or other pathological conditions.
The direction of flow is the same as that of the veins (from the periphery and the limbs toward the heart),but the speed of fluid movement within the lymphatic vessels is much slower. The force that propels fluid through the lymphatic vessels is a combination of small peristaltic contractions of the lymphatic vessel walls and the capillary phenomenon.
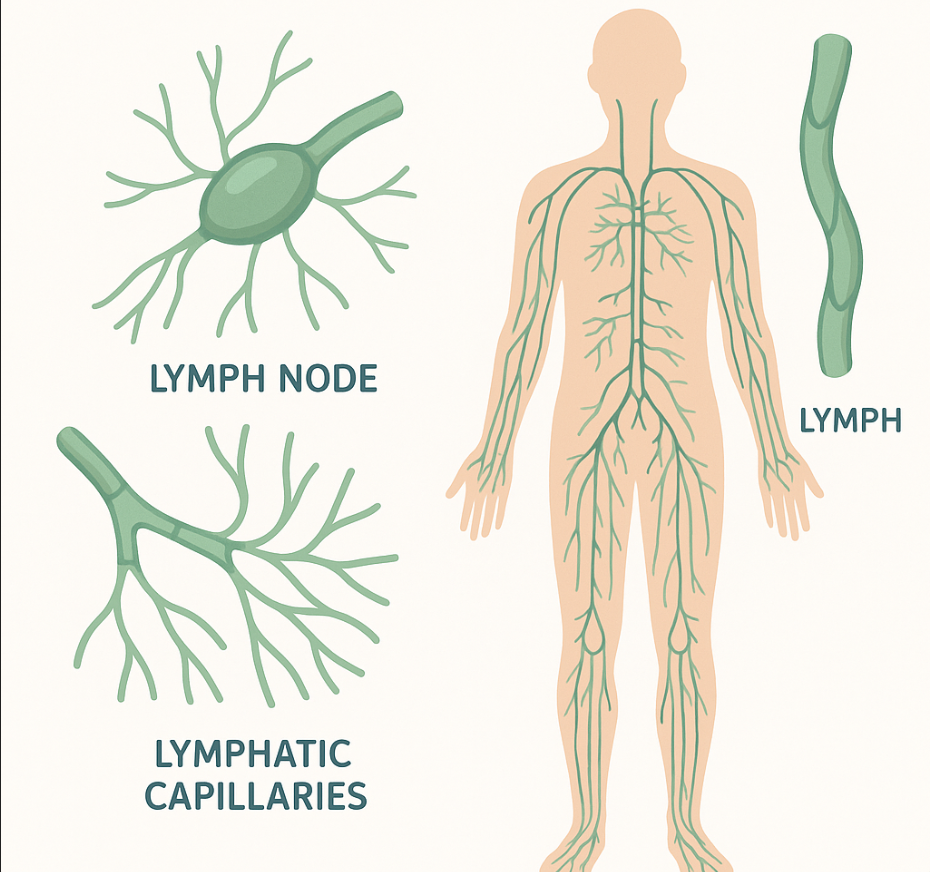
Lymph Nodes: The Defense Stations
Lymph, along its course, passes through intermediate stations called Lymph Nodes, where the immune system recognizes harmful external agents and initiates the body’s defense response. του οργανισμού. Groups of lymph nodes are found in the inguinal (groin) and axillary (armpit) regions, in the neck (cervical region), as well as within the thoracic and abdominal cavities. As lymphatic vessels approach the heart, they merge (converge), gradually increase in diameter, andultimately drain into the venous system at a site called the Venous Angle, located at the left subclavian vein.
Lymphatic Disorders
Lymphatic Disorders
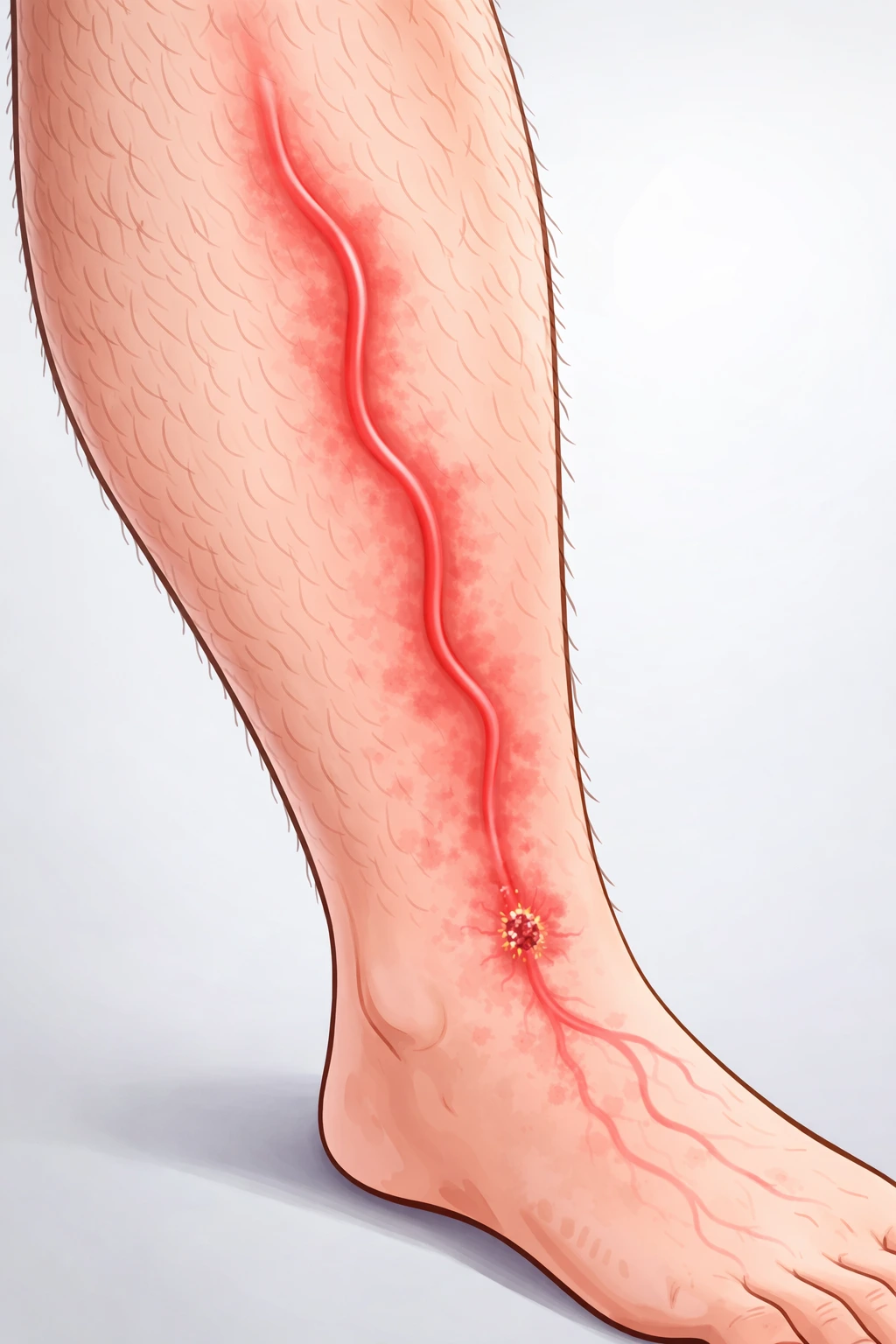
Infection of the lymphatic vessels (invasion by a microbial agent) causes inflammation known as Lymphangitis. It is characteristically accompanied by red streaks, tenderness, and fever. Quite often, lymphangitis is caused by or coexists with Cellulitis , which is a more generalized infection of the subcutaneous tissue (the tissue located between the skin and the muscles). This leads to diffuse redness, warmth of the affected area, fever (or low-grade fever), and the red streaks of lymphangitis may not always be visible.
Lymphangitis – Cellulitis
Lymphangitis – Cellulitis
Fever
High fever with chills
Redness
Red streaks on the skin
Pain
Painful affected area
Immediate Management
Management of Lymphangitis – Cellulitis
Treatment requires prompt evaluation by a specialist and timely antibiotic therapy to prevent irreversible complications such as lymphedema.
By a specialized physician
Immediate Evaluation
Timely administration
Antibiotic Therapy
Lymphedema prevention
Avoidance of Complications
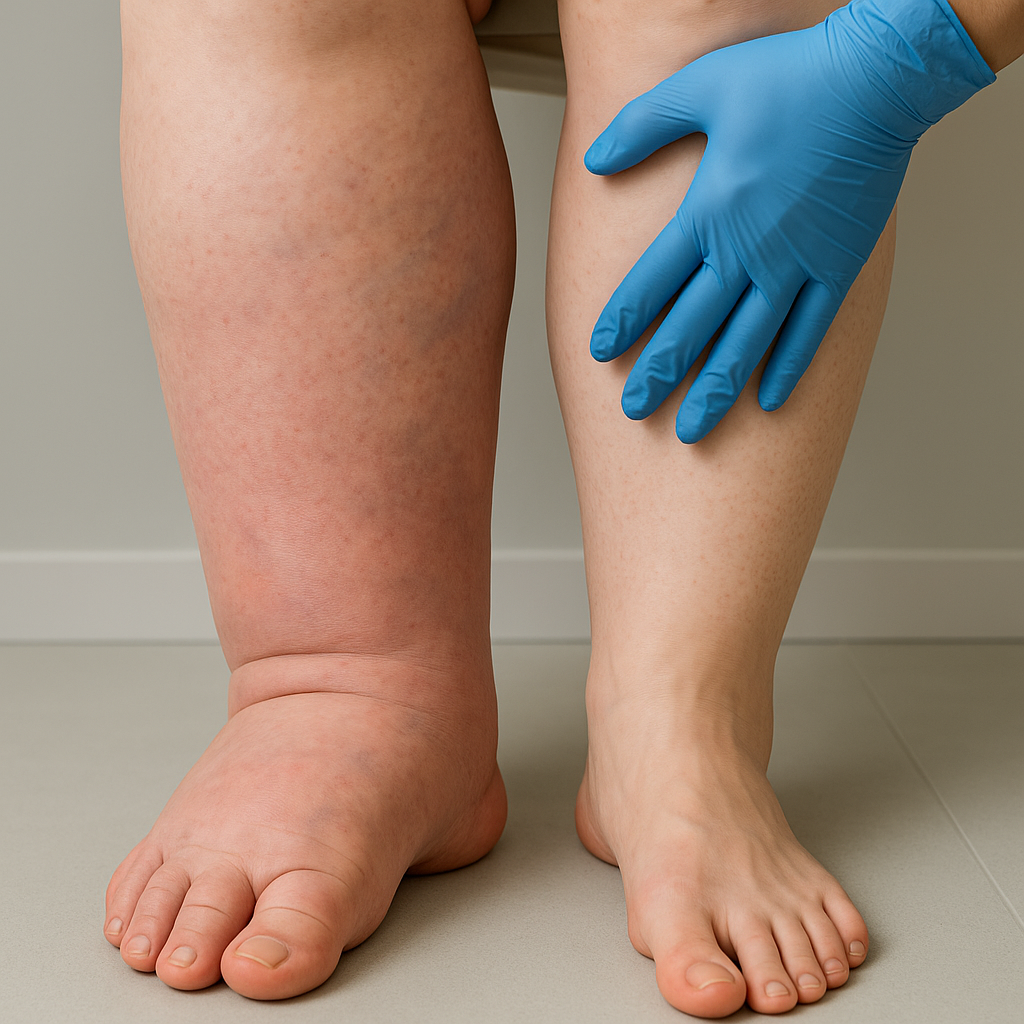
What is Lymphedema?
The Lymphedema is the accumulation of interstitial fluid in one or more parts of the body and may be due either to congenital agenesis (absence) of lymphatic vessels (Primary Lymphedema), or to dysfunction of the lymphatic vessels caused by an acquired factor (Secondary Lymphedema).
Primary Lymphedema
Congenital agenesis (absence) of lymphatic vessels
Secondary Lymphedema
Dysfunction caused by an acquired factor
Most Common Causes of Secondary Lymphedema
- Injury or surgical damage to the lymphatic vessels.
- Infection or inflammation of the lymphatic vessels.
- Tumors or lymph node metastases that obstruct flow.
- Removal of lymph nodes or radiation therapy in lymph node regions.
Chronic retention of lymph in tissues gradually leads to hardening, thickening of the skin, and worsening of the swelling if not treated.
Characteristics of Lymphedema
- Swelling that usually starts from the fingers or limb.
- Heaviness, tightness, and fatigue of the limb, especially at the end of the day.
- Hardening and thickening of the skin over time.
- Increased risk of skin infections.
Therapeutic Approach
Management of Lymphedema
The success of lymphedema treatment depends on the stage of the condition and should be assessed by the patient’s vascular surgeon.
Decongestive Manual Lymphatic Drainage
The cornerstone of lymphedema treatment is decongestive manual lymphatic drainage sessions (also known as lymphatic massage) performed by specially trained physiotherapists.
- Lymphatic Massage
Special Lymphedema Garment
Used in combination with a graded compression lymphedema garment (stocking or glove). Its role is to maintain the results of manual drainage for as long as possible.
- Graded Compression
Special Devices
Additionally, specialized devices that perform lymphatic massage are used, and their results can be comparable to manual drainage.
Surgical Techniques
The surgical techniques available for the causal treatment of lymphedema include lymphovenous anastomoses and lymph node autotransplantation.
The treatment of lymphedema requires a personalized approach and close collaboration between the patient and the treating physician to achieve the best possible outcomes.

